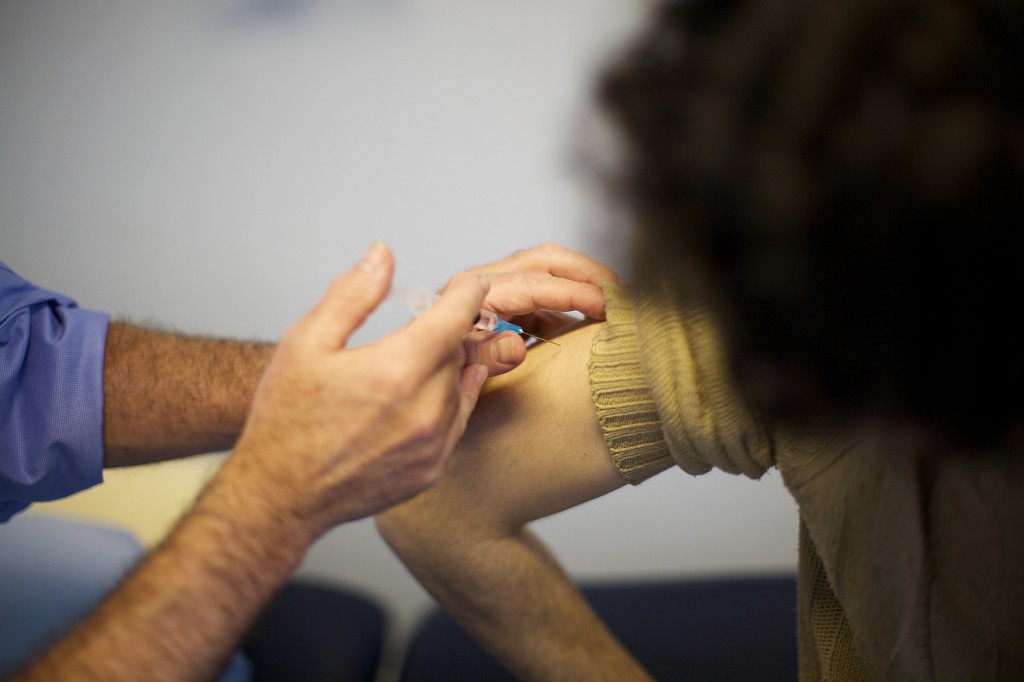
The COVID-19 vaccination programme is the biggest to have ever taken place in the UK. Over 48 million doses have now been administered, which is estimated to have prevented over 10,400 deaths in England up to the end of March.
Recently, there have been reports of an extremely rare condition involving blood clots with low platelets after vaccination. Although this condition remains extremely rare and unlikely to occur, it appears the risk exists between 4 days and 4 weeks after the first dose of the AstraZeneca vaccine is given.
The Joint Committee on Vaccination and Immunisation (JCVI) has considered evidence from the Medicines and Healthcare Products Regulatory Agency (MHRA) and has issued advice to the government on the use of the COVID-19 AstraZeneca vaccine.
The expert committee has weighed the balance of benefits and risks and advises that the benefits of vaccination with the AstraZeneca vaccine far outweigh the risk of this extremely rare condition for individuals 30 years of age and over and those who have underlying health conditions which put them at higher risk of severe COVID-19 disease. It’s important to remember that all medicines have risk, even aspirin. The risk of a blood clot with low platelets happening to you following vaccination is very low.
In this blog we take a look at the JCVI recommendations on the COVID-19 AstraZeneca vaccine.
What is the issue?
In recent weeks, there have been a very small number of reports from the UK and internationally of an extremely rare condition characterised by thromboembolic events (blood clots) accompanied by thrombocytopenia (low platelets) following the first dose of the AstraZeneca COVID-19 vaccination.
Around 8 people develop this condition for every million doses of the AstraZeneca vaccine given. This is seen slightly more often in younger people and symptoms tend to occur between 4 days and 4 weeks following vaccination.
Are there any conditions that make the chances of having one of these clots with low platelets more likely?
Currently, the data available do not identify any particular condition which leaves people at greater risk of these extremely rare adverse events – studies to fully understand adverse events are ongoing. It is currently advised that those who are clinically extremely vulnerable and at greater clinical risk from COVID-19, take up the offer of vaccination when invited as the risks to them if they get ill with COVID-19 are far greater than any risk from the vaccine.
Are women or men affected more?
Suspected cases have been reported in patients of all ages in men and women. Whilst reports from some countries have suggested a substantially higher number of cases amongst females, based on the events reported to the MHRA in the UK, such a distinctive gender difference has not been observed.
What is the advice for pregnant women?
The JCVI have advised that pregnant women are routinely offered vaccination against COVID-19.
There have been no specific safety concerns identified with any brand of COVID-19 vaccines in relation to pregnancy.
Real-world data from the United States shows that over 90,000 pregnant women have been vaccinated, mainly with mRNA vaccines including Pfizer-BioNTech and Moderna, without any safety concerns being raised.
Based on this data, the JCVI advises that it’s preferable for pregnant women in the UK to be offered the Pfizer-BioNTech or Moderna vaccines routinely where available.
What are the JCVI advising?
The JCVI recommendations are based on a careful assessment of the high level of protection against serious disease from COVID-19 (such as intensive care admission or death) provided by vaccination compared to the very small risk of this extremely rare blood clotting with concurrent low platelet (blood cell count) event. JCVI currently advises that it is preferable for adults aged under 30 years without underlying health conditions that put them at higher risk of severe COVID-19 to be offered an alternative to the AstraZeneca vaccine, if available.
The benefit/risk balance is more finely balanced in the youngest adults aged 18 to 29 years compared to older adults because the benefits from vaccination increase steeply with age. The advice to offer an alternative vaccine in this youngest adult age group is based on a careful assessment of the benefit/risk balance and made out of an abundance of caution and because an alternative vaccine is available for this age group.
The JCVI will continue to review data as they become available and will update advice where appropriate.
Find out more about the roles of the JCVI and MHRA.
Why isn’t use of the AstraZeneca vaccine being suspended?
Real-world vaccine effectiveness studies conducted in the UK confirm that the AstraZeneca vaccine works well in adults of all ages, providing high levels of protection from severe illness or death caused by a COVID-19 infection. The benefits of vaccination with the AstraZeneca vaccine still far outweigh the risks for the majority of the population.
The JCVI has closely monitored and reviewed data at every step of the vaccination programme and will continue to do so as each age group becomes eligible for vaccination.
This close scrutiny of the data continues to ensure that the vaccination programme is led by the most up-to-date data.
If I am under 30 with no underlying medical conditions and have had a first dose of AstraZeneca, should I not have the second dose?
To date there have been 4 suspected cases of this extremely rare adverse event following the second dose of the AstraZeneca vaccine. The majority of people who were offered the first dose of the AstraZeneca vaccine should continue to be offered the second dose, irrespective of age – anyone who suffered severe adverse effects following the first dose should seek advice as they may need to be offered an alternative vaccine in some cases. The JCVI will continue to review data as they become available and update this advice as required.
What about if I have conditions that require special precaution?
For those who have conditions that require special precautions for use of the AstraZeneca vaccine (as listed in the updated MHRA information for UK healthcare professionals), then do as follows:
- When you present for vaccination you will be asked about additional risk factors, using the materials provided. If you are at increased risk, you should have a discussion about the benefit and risks of receiving the AstraZeneca or other vaccine with your doctor.
- If, following a conversation with a doctor, you choose to go ahead with the AstraZeneca vaccination, vaccination sites should make this option available.
- If you want an alternative vaccine, the NHS will put appropriate arrangements in place.
If I am under 30 with no underlying conditions, can I choose to get the AstraZeneca vaccine anyway?
While the JCVI recommends that it is preferable that under 30s are offered an alternative vaccine if available, individuals can choose to have the AstraZeneca vaccine.
To make an informed decision it is important that all individuals are provided with the relevant information, including the benefits and risks, and that they have the opportunity to discuss this with their healthcare provider if they wish.
What side effects do I need to look out for after the COVID-19 vaccine?
Although serious side effects are very rare, if you experience any of the following from around 4 days to 4 weeks after vaccination you should seek medical advice urgently:
- a new, severe headache which is not helped by usual painkillers or is getting worse
- a headache which seems worse when lying down or bending over or
- an unusual headache that may be accompanied by: blurred vision, nausea and vomiting, difficulty with your speech, weakness, drowsiness or seizures
- new, unexplained pinprick bruising or bleeding
- shortness of breath, chest pain, leg swelling or persistent abdominal pain
Please note we are unable to provide clinical advice to members of the public or respond to individual health concerns. Please contact your GP or NHS 111 or visit www.nhs.uk. Only urgent non-clinical enquiries should be made by phone.
View original article
Contributor: Blog Editor