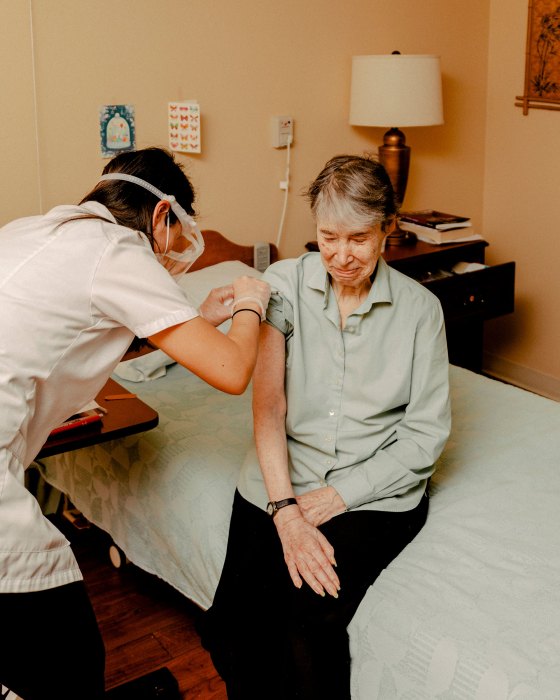
On a frigid morning in January, Trudy Ronnel settled into her favorite sofa chair at the Westminster Place senior-living community in Evanston, Ill., pulled down the neckline on her red blouse and braced herself for a shot she’d anticipated for almost a year. At 92 years old, with multiple medical conditions, she spent most of 2020 fearful of contracting the COVID-19 plague that ravaged the world outside her first-floor window.
To protect herself, for the past few months she’d avoided Westminster’s communal rooms, which had provided a means to stay active and engaged but risked becoming a pathogenic petri dish.
Whenever she left her room, she dutifully wore a surgical face mask and maintained the mandated 6-ft. distance. The most difficult change came in the fall, when visits from her son, daughter and five grandchildren were cut off.
Living in relative isolation was not how Ronnel envisioned spending her golden years. Like millions of Americans, as soon as the first coronavirus vaccine was authorized, she began anxiously counting down to the day she’d receive her shot. As an elderly resident of a long-term-care facility, Ronnel is at higher risk of getting infected and experiencing serious symptoms, and thus belongs to one of the first priority groups to get vaccinated, along with health care workers. So, when a Walgreens pharmacist finally appeared in her doorway with the shot on Jan. 6, it came as a welcome sight. After getting the injection, Ronnel allowed herself to feel something that she hadn’t felt since the pandemic first began: the prospect of normality. “I hope this all begins to end soon,” she says.
That will depend. TIME spent the past year observing, traveling and speaking with dozens of people involved in the development, distribution and administration of the coronavirus vaccine. A month into the operation it has become clear that health experts, military logisticians and government authorities have often been at odds with one another over miscues, miscommunications and mistrust as they grappled with overcoming a tangle of logistical challenges in building an unprecedented health campaign from scratch.
According to local health officials, the Trump Administration’s decision to limit the federal government’s role in administering the vaccines left each state to create its own plans for locally distributing the shots and launching programs for getting them into people’s arms. That already-complicated logistical task, they say, was compounded by a lack of funds and a health care workforce already overwhelmed with COVID-19 testing, contact tracing and pandemic-control campaigns, not to mention mixed messages that left states in the dark about how many doses they could expect, and when.
In rolling out the vaccine, the U.S. in many ways repeated the same mistakes it made with COVID-19 testing last spring. Lack of federal leadership first in coordinating distribution of the tests, and later in supporting states to set up and staff testing sites, led to limited access and critical delays in getting results. Public-health officials across the country, as well as many experts TIME spoke with, say there has been a similar lack of coordinated planning and infrastructure to distribute and administer vaccines at the local level. “This vaccination program is complicated, and the way it’s gone so far is a microcosm of the 11 months of failed federal response,” says Dr. Tom Frieden, former director of the Centers for Disease Control and Prevention (CDC) under President Barack Obama. “There has been a lack of organization, a lack of a systemic approach and a lack of a public-health approach coming out of the White House.”
The Biden Administration enters office exactly a year into the U.S. pandemic, with the country’s tally of COVID-19 cases at 24 million, along with 400,000 related deaths. Those numbers are only growing. The Administration’s new health leaders will come in with their own ideas for how to control the pandemic and answer the critical question of what went wrong. Their answers won’t simply be a matter of administrative accountability, but a matter of public health and economic urgency. If the current slow pace of getting vaccines from the assembly lines into people’s arms continues, it could lead to weaker population-level protection, enabling the virus to continue spreading–especially with a new, more contagious variant afoot. And the more it spreads, the more likely it is that new, mutant forms will emerge, some of which could be resistant to any hard-won protection from vaccines. Health officials warn that current delays and problems in moving vaccines will only be amplified when tens of millions more Americans become eligible for COVID-19 shots in coming months.
Biden’s team has indicated it will erase the brand name Operation Warp Speed (OWS) from the federal vaccine initiative, and introduce a new structure with the immediate goals of vaccinating 100 million people by the 100th day of his presidency while working toward reopening most schools by spring. Getting there will require a more aggressive federal response to support states, the President says, involving the National Guard and the Federal Emergency Management Agency to set up thousands of mass-vaccination centers and mobile teams to reach people living in more remote areas. Whether these efforts will be enough to efficiently immunize hundreds of millions of people in a matter of months will depend on how well the Biden Administration, in contrast to the Trump White House, can persuade the public to trust the science behind the vaccines, and the public-health experts who maintain that until most of the population is vaccinated, the virus will retain the upper hand.

The only way out of this pandemic, public-health officials say, is to use vaccines to achieve herd immunity, a type of biological fortress in which the vast majority of the population is protected against disease, blocking a roaming virus from finding new human hosts. The U.S. authorized two vaccines in mid-December: the first from Pfizer-BioNTech and the second from Moderna, both roughly 95% effective in protecting against the disease. The government-led effort to develop and test COVID-19 shots stands as a record-setting feat that reduced standard vaccine development time from 10 years to under one (and there are a handful of others currently in testing).
But having an authorized vaccine isn’t the same as having a vaccinated public. Getting the shot to some 300 million Americans was never going to be trivial, but Donald Trump’s Administration fell well short of its projections. The Trump team had boasted that by Jan. 1, 2021, some 20 million Americans were expected to be vaccinated against COVID-19. Instead, when the New Year rang in, just 3.5 million people had received the shot.
The quest to develop and manufacture a safe and effective vaccine for a new infectious disease was always going to be a gamble, even for pharmaceutical companies with deep experience in mass-producing vaccines. To motivate the industry, the Trump Administration established OWS, a so-called whole-of-America public-private partnership that coordinated pharmaceutical leaders, government health experts and the military to incentivize and pave the way for developing COVID-19 vaccines as quickly as possible. The White House compared the crash program, in its size and scope, to the Manhattan Project, which produced the world’s first atomic bomb that helped end World War II.
By the spring, billion-dollar contracts were drawn up to support the research-and-development and manufacturing costs for millions of doses from Moderna, AstraZeneca, Novavax, Sanofi-GlaxoSmithKline and Johnson & Johnson. Pfizer-BioNTech chose not to accept support from OWS to develop its vaccine but signed a nearly $2 billion contract to supply 100 million doses with an option for 500 million more even before its vaccine received federal approval. To lead the group, Trump chose Moncef Slaoui, the former head of research and development for pharmaceutical giant GlaxoSmithKline, who had brought 14 vaccines to market over his career.
The creation of a vaccine was just one item on a long list of needs. Inoculation on such a mass scale meant truckloads of supplies had to be located and obtained–little things like glass vials to hold the vaccines, alcohol pads, masks and other personal protective equipment for people giving the shots. To oversee logistics, Trump tapped Gus Perna, a four-star Army general who spent his career working to ensure that soldiers stationed in the world’s most hard-to-reach places were still able to get food, fuel, weapons and supplies. Perna quickly handpicked his staff–the best officers and civilians he’s worked with over the past 37 years–and familiarized himself with the practices, players and perplexing jargon of this new unfamiliar terrain of public health.
The national COVID-19 vaccination campaign is an unlikely collaborative effort led by the Department of Health and Human Services (HHS) and the Department of Defense out of a low-rise Brutalist office building in the shadow of the U.S. Capitol in downtown Washington, D.C., where HHS is headquartered. From the start, the military’s regimented, top-down approach clashed with the more casual culture at HHS, particularly at the CDC. Many at the agency had a difficult time understanding why Trump was bringing in soldiers to carry out a core CDC mission: controlling a disease. For decades, the CDC has been managing, without major issues, the Vaccines for Children Program, the country’s largest vaccination initiative–working with manufacturers and distributors to determine supply and storage of more than a dozen childhood immunizations, and collaborating with states to oversee shipment of the shots. Dr. Nancy Messonnier, director of the CDC’s National Center for Immunization and Respiratory Diseases, which researches vaccine-preventable diseases and works with CDC committees to set national policies on any vaccines distributed in the U.S., including childhood immunizations, repeatedly pushed back against the Pentagon’s taking the driver’s seat. She made it clear during conference calls with OWS that she and her team felt it already had a solid vaccine-distribution plan in hand, based on one that had been drawn up to deal with the H1N1 swine-flu pandemic in 2009.
But when Perna began establishing daily “battle rhythm” meetings between federal agencies and health-industry leaders to discuss the latest progress or problems with the vaccine program, they were led by HHS and the military, not by CDC, as the agency had done during previous outbreaks. Weekly phone conferences with states, broken into groups by region, were also arranged by OWS to ensure public-health leaders had the latest information and could ask questions. Although CDC had a seat at the table, agency officials felt they were consistently sidelined. (The agency did not respond to requests for comment on this story.)
OWS officials determined CDC’s plans were old and not nearly extensive enough to accomplish the mass vaccination they were faced with. In the end, though, OWS contracted with McKesson, a private health care distribution company CDC had used since 2006 to get its childhood vaccines around the country. McKesson subcontracted the work to logistics behemoths such as UPS and FedEx. OWS also created partnerships with pharmacy retailers, such as Walgreens and CVS, to administer vaccines to residents and staff at long-term-care facilities. Overall, OWS has spent nearly $25 billion in federal funding to more than 120 companies to develop, manufacture and deliver vaccines across the nation. Authority under the Defense Production Act was invoked 18 times to mobilize U.S. private-production capacity to manufacture the supplies. Much of the material wasn’t even in the U.S. For example, Goldbelt, an FDA-authorized company that manufactures in China, was granted a $125 million contract to deliver 530 million needles and syringes.
The blueprint for the national strategy is represented in a dozen maps and charts Scotch-taped to the walls of Perna’s seventh-floor office at HHS headquarters. And yet, despite the attention to detail and months of strategizing, he acknowledged that success is far from certain. “Our vulnerability will be: we’re too confident,” he tells TIME. “So we have to constantly check ourselves and ensure the plans work and make sense.”

As the delivery truck snaked its way over Northern California’s interstates and two-lane highways on Dec. 15, a team of distribution analysts in Washington, D.C., watched over nearly every aspect of its journey in real time. They could see the stops the driver took, they knew the weather outside and, most important, they knew the condition of the precious cargo onboard: thousands of doses of COVID-19 vaccine.
In the back of the truck, containers packed with vials of Pfizer-BioNTech’s newly authorized vaccine were loaded onto customized trays, resembling small pizza boxes, each container carrying at least 975 doses. The containers were also packed with dry ice, tracking devices and sensors, which enabled the team to watch as the temperatures of two of the trays–one destined for Napa, Calif., the other to Sonora, Calif.–plunged to –133.6°F, more than 21° below the accepted threshold. A call was made to the truck driver to stop and keep the trays in the vehicle.
Thousands of doses of vaccines made by Pfizer-BioNTech and Moderna have been wasted since shipments began in early December, according to government officials. The reasons vary–sometimes doctors inadvertently leave vials out too long; sometimes the day ends with doses that were supposed to be administered left over because patients never showed–but several deliveries have encountered temperature problems.
If the doses deviate from their target destination in each of the nearly 42,000 U.S. ZIP codes, or if the temperature of the vials exceeds –76°F (–60°C) or falls below –112°F (–80°C), officials at Pfizer-BioNTech and the government are immediately alerted. “We want to see everything,” says Marion Whicker, who spent decades moving tanks and armored vehicles around war zones for the Army and now serves as OWS’s head of logistics for vaccine distribution. “Just like you track your Christmas gift from Amazon.”
The information streams into the Vaccine Operations Center, known as the VOC. The windowless, conference-hall-size command hub at HHS headquarters is where uniformed military members, HHS officials, private contractors and U.S. marshals keep a watchful eye over logistics. On the operations floor, dozens of analysts work behind rows of computer monitors. Along the far wall in front of them, four large flat screens glow with real-time information about the day’s deliveries, which enables them to track shipments from manufacturing facilities to their destinations across the nation. But once the vaccine vials leave OWS’s hands, the daunting task of distributing the shots to the people who need them falls to the states.
Already facing shrinking budgets and overwhelmed by the demands of managing the pandemic over the past year, state public-health departments have struggled with the additional obligation to distribute and administer vaccines. Last fall, the CDC asked every state health department and jurisdiction the agency supports for a plan; most were vague by necessity and in some cases relied too heavily on existing programs and call centers designed for childhood-immunization programs, but which may not have been robust enough to handle COVID-19. “They underestimated the uniqueness of vaccinating 30% of Americans in a few months,” says Joshua Walker, co-founder of Nomi Health, which helped the health departments of Iowa, Florida, Nebraska and Utah set up COVID-19 testing programs and is now supporting dozens of cities, counties, states, hospitals, airports, hotels and other groups to quickly manage vaccination programs.
In addition, many states found that initial federal funding for COVID-19-related response wasn’t adequate, making it hard to form concrete plans to buy the ultra-cold freezers needed to store the Pfizer-BioNTech vaccine, for example, or to hire staff for vaccination clinics. Funding for COVID-19 response authorized by Congress last spring expired at the end of the year, says Dr. Jinlene Chan, acting deputy secretary for public health services for the Maryland department of health, and “we had no anticipation of any additional dollars of support for all of these efforts.” As the number of cases in her state started to climb, and to ensure that citizens would get vaccinated, Chan says, other pandemic-related efforts, like the depth of the contact-tracing interviews, had to be temporarily scaled back to prioritize vaccination. As Kris Ehresmann, director of infectious disease at the Minnesota department of health, puts it, “We got an amazing vaccine, the Cadillac of vaccines, and yet we’re skimping on resources for getting it out.” New funding to support state COVID-19 programs was authorized only in the last days of 2020.
On the weekly calls, Perna and Slaoui informed state health officials that the federal government would get them the vaccine but that it was up to them to work with the CDC in order to form and execute “last mile” inoculation plans. “We’re solving problems ahead of execution,” Perna said on one call, observed by TIME in early December. “Does this mean perfection? No. The plan is only good to get you started. What’s important is the open collaboration and communication between everyone.” To keep track, a government contractor developed a new software platform called Tiberius, which enables states and federal agencies to see their orders and track vaccine shipments. After vaccine producers say how many doses are available for distribution in the upcoming week, each state then has the opportunity to place an order up to a certain amount allocated by OWS. Once approved, that order is locked into Tiberius every Tuesday.
Even with the system, states at first complained they didn’t know exactly how many doses they could expect. Some say they expected a certain amount based on what the federal government had told them (which Perna says were based on rough population-based estimates) only to find out just the day before delivery–or sometimes on the delivery day itself–that they’d be getting fewer than anticipated. That made it nearly impossible to adequately plan vaccination campaigns. Dr. Eric Dickson, CEO of Massachusetts’ UMass Memorial Health Care, says his hospital system received half the number of doses it expected during the first two weeks of vaccinations, which led to “vaccine envy” among staff members who could not get vaccinated along with their colleagues. Though the situation has improved since then, Dickson says communication from the federal government was sorely lacking at first. “It could have been a lot better than going to the loading dock with the FedEx guy and saying, ‘How many did we get?’”



The COVID-19 vaccines authorized so far, from Pfizer-BioNTech and Moderna, require two shots spaced about a month apart. In the initial push, OWS sent out the first dose but held back a reserve of second doses, because Perna did not want to be caught shorthanded if manufacturing faltered and supply dried up. Vaccinemakers, however, have proved their reliability. A steady stream of more than 4 million doses were available for distribution for each of the past three weeks.
Because of that, on Jan. 8, Biden’s team announced that it planned to release nearly all available vaccines in order to inoculate as many people as possible, rather than hold vaccines back to ensure that anyone who received a first dose would get the second one. It didn’t take long before the Trump Administration said it would adopt this immediate distribution system–but states expecting an additional windfall of vaccines were frustrated to learn on Jan. 15 that the government did not in fact have vaccines on reserve to release. The discovery was neither the first nor the last disappointment states would face as the rollout unfolded.
Amid the chaos and confusion, many states simply aren’t administering the shots delivered to them. Though the pace is picking up, CDC data published Jan. 19 show only about 15.7 million doses have been administered, out of 31.1 million delivered to the states. Some of the shortfall may be a reporting lag as states learn new tracking systems. Another possible factor is winter storms delaying some deliveries and forcing office closures. But it’s clear there are entrenched problems.
States don’t have the staff or infrastructure to manage the volume. When Florida’s Miami-Dade County opened up 2,000 or so vaccination appointments, they were gone in under a minute as 80,000 people slammed the reservation site during those 60 seconds. Believing that their existing childhood-vaccination programs could handle the load, many states failed to fully account for the overwhelming demand from a desperate and impatient public. County health offices around the country are inundated daily with phone calls from residents bewildered by the mixed messages from federal, state and local officials.
Vaccine eligibility requirements have contributed to that confusion. Though the CDC provides recommendations about who should get the shots first, states make their own rules. For example, New York began vaccinating all people over age 65 on Jan. 11, while in Maryland, that group is set to gain eligibility on Jan. 25. Such differences are causing potentially dangerous confusion that could lead some to miss their opportunity for a shot or decide not to get one at all.
Making matters worse, once a vial (which contains at least five doses in the case of the Pfizer-BioNTech vaccine and 10 doses in the case of Moderna) is opened, it needs to be used within six hours or discarded. As a result, in situations where someone changes their mind about getting vaccinated or misses an appointment, nurses, doctors or pharmacists, holding doses that would otherwise go to waste, are deciding to give them to anyone who happens to be around–regardless of whether they are in the right priority group. This, in some cases, has become regional policy; Michigan’s chief medical executive, Dr. Joneigh Khaldun, says she has told providers to aim to use 90% of their vaccine supplies within seven days of receiving them, even if that means straying from state guidelines in “a good-faith effort to use the vaccine.”
The lack of federal leadership has resulted in state health departments scrambling to figure out solutions, creating a patchwork approach to allocating and administering allotted doses. Health officials in Florida decided to offer a number of vaccines through Eventbrite, a website primarily known for obtaining tickets to sports events, concerts and even monster-truck shows. In southwest Florida’s Lee County, officials decided against building an appointment-based system, so senior residents instead had to spend more than seven hours, some overnight, in line, hoping to snag one of the limited vaccines available. “It’s only now that the states are starting to realize the gravity of the situation and the volume required to vaccinate their populations,” says Dr. Peter Hotez, a vaccine scientist from Baylor College of Medicine in Texas.
Given the diverse population and topography of the U.S., and the differences from state to state, local health departments are trying to come up with creative and flexible strategies to reach people in as short a period of time as possible. In Alaska, for example, health workers have been taking planes, boats and sleds to reach the 80% of the state’s communities living in places that cannot be accessed by road, and setting up makeshift clinics inside bush planes or going door-to-door in villages to vaccinate Indigenous communities. And because of the travel challenges, the state requested and now receives its allotments for these groups from the Indian Health Service (IHS) monthly rather than every other week, so doctors and nurses can plan in advance, and distribute and use the vaccines more efficiently.
In Carlton County, Minnesota, health officials plan to rely on drive-through vaccination clinics to make the process more convenient. After months of planning, the county’s drive-through clinic opened for two days in December to vaccinate first responders; the health team plans to reopen it soon, along with a number of other drive-through locations, to accommodate all of the county’s residents when it’s their turn to get the shots. “The drive-through model allows us to potentially vaccinate thousands of people in a day,” says Ali Mueller, emergency-preparedness coordinator for the county. Other states have taken similar approaches, such as converting professional sports stadiums into mass-vaccination sites, some of which operate 24/7.
Carlton County also worked with Redlands, Calif.–based Esri, a geographical information systems software company, to set up a tracking tool that offers real-time information on the ebb and flow of people through the county’s drive-through clinic. In theory, that will help Carlton’s health team anticipate what times of day demand will likely be highest at their next clinics, so they know ahead of time how many vaccines they will need and thus don’t waste any doses. Many other states and counties are working with similar companies to build software to manage the higher demand and to answer people’s questions about where and when they can get vaccinated.
Without solutions to such challenges, the national vaccination effort will only grow more difficult in the coming weeks. After all, health care workers and long-term-care residents are both fixed populations that are relatively easy to locate; when vaccines are opened up to everyone in the country, things could rapidly deteriorate into an even more chaotic state than they are in today.
It’s difficult to say whether this is a uniquely American problem. Some countries, such as Israel and the United Arab Emirates, have outpaced the U.S. in vaccinating more people out of every 100–about 32 and 20, respectively, compared with less than five in the U.S. In Israel, that success can be traced to a combination of centralized vaccination programs and saturated messaging campaigns to educate people about the public-health benefits of vaccines and encourage them to get immunized. In contrast, rollouts in European countries have been slower, partly because the E.U.’s regulatory agency lagged behind both the U.S. and the U.K. in authorizing the first shots.
What we do know is that vaccinating the general public in the U.S. will take more of everything that has been in short supply during the first phases of rollout: vaccines themselves, storage for those doses, facilities that can accommodate mass vaccine clinics, staff or volunteers to run them, and communication with people who will ultimately receive the shots.
More doses are on the way. Not only are Pfizer-BioNTech and Moderna perfecting their manufacturing and distribution systems, but other vaccine candidates are moving closer to emergency-use authorization, perhaps getting the green light as early as next month. The crucial challenge will be ensuring that as supply ramps up, so too does the machinery of vaccination. While each state has its own challenges and considerations to make, the federal government can even the playing field by ensuring each one has the resources and information required to implement a system that works at the local level. To actually turn vaccines into vaccinations, states also need support and transparency from the federal government; enough money to furnish a robust network of well-staffed public vaccination centers; and coherent public-information campaigns, both for building trust in COVID-19 vaccines and for conveying who is eligible to get vaccinated, when and where.
Biden plans to address those weaknesses and change the current pace of the U.S. vaccination program. “The vaccine rollout in the United States has been a dismal failure, thus far,” he said in a Jan. 15 speech. He’s already asked Slaoui to submit a letter of resignation from leading OWS scientific development. Internally, officials with OWS expect further personnel changes in the weeks to come, although–for the time being–the Biden team plans to keep Perna in his current role.
Meanwhile, Biden’s proposed plan does indeed give the federal government a more central role in ending the pandemic, which includes establishing more federally funded and operated vaccination sites. “On my first day in office,” he said, “I’ll instruct the Federal Emergency Management Agency, FEMA, to begin setting up the first of these centers,” he said in that speech. He set a goal of standing up 100 such sites by the end of his first month in office. To get this done, Biden has proposed a coronavirus-relief package that calls for at least $20 billion for vaccine distribution and additional funds to support the hiring of 100,000 public-health workers. If approved by Congress, that could significantly relieve the burden on cash-strapped states with exhausted health care workforces. Biden has also promised “a massive public-education campaign” to address another major roadblock in the quick administration of vaccines: rebuilding trust among people who have been hardest hit by the pandemic, in racial and ethnic minority groups including Black, Latinx and Indigenous Americans.
As the rollout continues, more vaccines are administered each week, and many states are falling into a rhythm of knowing how many vaccines to expect on a regular basis. But each day the demand far exceeds the supply of shots is a day the virus can gain the upper hand by infecting more people, sending them to the hospital or contributing to their deaths. Vaccines can lead us to the end of the pandemic, but only if we find a way to move them more efficiently from the government’s hands and into the arms of Americans.
With reporting by Alejandro de la Garza, Simmone Shah and Leslie Dickstein
View original article
Contributor: W.J. Hennigan, Alice Park and Jamie Ducharme