The new, heavily mutated variant of SARS-CoV-2, Omicron first detected by scientists in South Africa, has put the public health community worldwide on high alert and the public on edge. Since then, evidence has mounted that the variant is highly transmissible. It is far more transmissible than, and is coming to predominate over, its immediately preceding variant, Delta. Omicron’s doubling time—how long it takes for the number of coronavirus cases to double—is just two to three days.
The first indications from South Africa are that infection with the Omicron variant may have milder consequences than infections with previous variants, especially in vaccinated people. Despite some claims, it’s premature to conclude that Omicron will cause mild illness with few consequences. For example, in South Africa’s Omicron wave, infected people have tended to be younger than in previous waves, and we know that younger people are more likely to have more mild disease when infected with any SARS-CoV-2 variant. And given the time lags between infections, hospitalisations, and deaths, it is still too soon even for South Africa to pick up a signal in its excess death monitoring system, one of the few real-time such systems among low- and middle-income countries (LMICs). Omicron is coming at us fast, but its full impact will take time to become apparent.
[time-brightcove not-tgx=”true”]
How did high-income countries respond to the news? Unfortunately, with knee-jerk travel bans rather than anything that might be mistaken for a coherent public health response.

Punishing South Africa for alerting the world to a new variant of concern is exactly the wrong way to be dealing with Omicron. The only effective response is global action and solidarity. Unfortunately, examples of both have been thin since the pandemic started. Omicron has so far been detected in 63 countries, and is surging in many of them. There is preliminary evidence, including from South Africa and the United Kingdom, that COVID-19 vaccines are less effective against Omicron than against Delta in preventing illness. The good news is that emerging data show that a booster dose restores high levels of vaccine effectiveness. The bad news is that too many people in the world have not had any doses of vaccine at all. We will need strategies worldwide to enhance vaccine equity and access and to scale up other protective measures alongside vaccines. Early evidence also suggests that unvaccinated people who have been infected with the virus in the past are not well-protected against Omicron—re-infection appears to be common.
Given all of these initial data, the World Health Organization (WHO) calls Omicron a “high risk” variant that could lead to further surges worldwide with severe consequences. What might these surges look like?
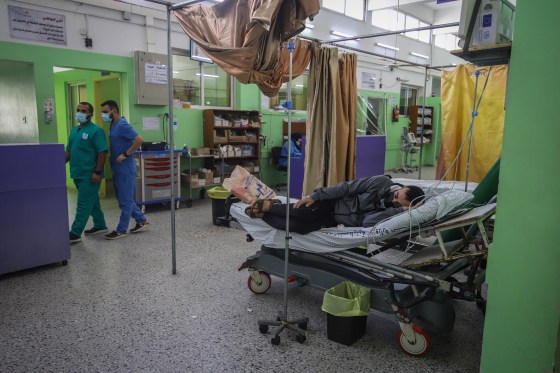
A massive spike in cases worldwide could be hugely disruptive and could lead to increased deaths. Even in the best-case scenario in which Omicron causes a mild illness, the repercussions could be huge. Imagine, for example, that the entire world caught a cold at the same time. There would be a rise in deaths among older, vulnerable people—such as those in nursing homes—and the mass absences from work would have major societal consequences. Even if only a small percentage of people get ill or die, a small percentage of a very large number would still be a large number. And in many nations, including the U.S., there is no slack in the health system to deal with another surge in COVID-19 hospitalizations. Hospitals are already at capacity dealing not just with COVID-19 (cases and deaths from Delta are rising in the U.S.) but with catching up on a backlog of surgeries and other treatments delayed or deferred by the pandemic.
Yet, there is no need for fatalism. Unlike the start of the pandemic, we now have a wide range of science-based tools that we can and must marshal.

In the face of the Omicron risk, the number one priority for all countries is to vaccinate the unvaccinated, especially those at highest risk: older adults, health care workers (including those who work with and care for the elderly in care homes), and people with underlying health conditions. As the WHO notes, “vaccines are likely to have some effectiveness against Omicron, particularly for severe disease, even if the performance is reduced compared with other variants.” Globally, the brunt of illness and death will fall on LMICs, where very few people have been vaccinated. Only 7.5% of Africa’s population are fully vaccinated.
After an exceedingly slow start, the supply of vaccines to LMICs has increased in recent months, and some middle-income countries in particular have been able to achieve good vaccination coverage. But there’s still much to be done to expand vaccine access. Rich nations should urgently donate doses to initiatives such as the African Vaccine Acquisition Trust and COVAX that are vaccinating populations in LMICs. So far, such donations have been miserly, ad hoc, and unreliable. Rich nations have also pre-purchased way more doses than they can ever use and should redirect the excess to LMICs immediately. Alongside donations, rich countries and vaccine companies must stop blocking LMICs from making their own doses. Omicron will hopefully spur the rich world to finally share vaccine patents and manufacturing know-how and support the globalized manufacture of doses.
In the United States, 3 in 10 people have not even had one vaccine dose. Political partisanship in the US is unfortunately the single most important predictor of vaccination status, with Republicans much less likely to be vaccinated than Democrats, so we will need Republican leaders to advocate that the unvaccinated get their shots. Given the emerging data that a booster dose improves vaccine effectiveness, getting boosters urgently to high-risk people, such as health workers, incarcerated people, and nursing home residents, is crucial. Staff working in these settings must also be vaccinated. Since nursing home staff can spread coronavirus to residents, and given that low vaccination rates among staff are linked with higher rates of infection and death among residents, there’s a strong case for mandatory staff vaccination in these settings and regular rapid tests to prevent the virus being introduced to them.
But a “vaccine only” strategy will not be enough to blunt the force of Omicron and prevent spikes in hospital admissions. We need “vaccine plus”: a surge of other evidence-based measures, alongside vaccines, to match the surge of SARS-CoV-2. We need a comprehensive public health strategy.
Governments should make available free rapid antigen tests (as has been done in the UK) and high-filtration masks to all households, even by mail. A positive rapid test shows you are infectious to others, which gives you the knowledge to stay home and help break the cycles of transmission. Visitors to high-risk settings, such as nursing homes, should do a rapid test and not visit if the test is positive. In addition, physical distancing, ventilating indoor spaces, hand hygiene, avoiding crowds, and reducing one’s number of social contacts can also help to control transmission of the more transmissible Omicron variant. In the U.S., the same partisanship that has influenced vaccination uptake is likely to also influence adoption of these other prevention measures, so we will need Republican governors and mayors to do their part to help protect their constituents. We need a collective, non-partisan, public health response. The virus doesn’t care how you vote.
We cannot know, of course, whether Omicron will be the last variant of concern. Another one could be around the corner. There would be much less anxiety, however, about any new variant if we had a “joined up” global health program in place: preparation can allay panic.
Our goal must be to reopen society in a way that does not cause mass illness and death. SARS-CoV-2 is not going to be eradicated, and we need to plan and prepare for what lies on the other side of the current Omicron wave. We can aim for a situation in which COVID-19 still circulates but there is much less transmission and much less severe illness, hospitalizations, and deaths, perhaps with seasonal peaks—a scenario akin to influenza. For that to happen, we’re going to need to vaccinate and boost the vast majority of people worldwide.
If we can achieve that, and with Omicron as the dominant variant globally, in most cases getting infected would cause no symptoms or just mild ones, requiring just a few days off work. Perhaps you’d wear a mask for a few days to protect others when you returned to the office. But in this scenario, one will be placing co-workers, and—indirectly—their families, at near-negligible risk of death. It is too soon to know whether three doses of vaccine will be enough to provide lasting immunity or whether, as with the influenza vaccine, we’ll need an annual shot (potentially tailored to specific strains). There may continue to be localized outbreaks, especially in places with low vaccination rates, requiring local use of measures like masks and distancing to drive down transmission and to protect the vulnerable.
Omicron is coming fast. We hope that it causes just a mild illness, but even this outcome could have massive health and societal impacts worldwide. Don’t forget the great majority of people infected in the pandemic to date have experienced mild illness, and yet the virus has already killed about 800,000 in the U.S. alone. Omicron is teaching us a lesson: our only way out of this pandemic is through global, not national, action, to immunize and boost the world while also using other public health measures to drive down transmission and protect health systems. Omicron will be a harsh teacher. It remains to be seen if we can finally be good students.
View original article
Contributor: Gavin Yamey, William Hanage and Tom Moultrie
